Lower Leg Injury Resource Center
Tibia Fracture
Symptoms, Causes, Treatments, Surgery and Recovery

Kevin D. Martin, DO, FAAOS
Orthopedic Foot and Ankle Surgeon
Associate Professor of Surgery
About the author – Dr. Martin specializes in orthopaedic surgery of the foot and ankle. In addition to his practice Dr. Martin serves as committee member of the American Orthopaedic Foot and Ankle Society and is a regular contributor to multiple medical journals including Foot and Ankle International.
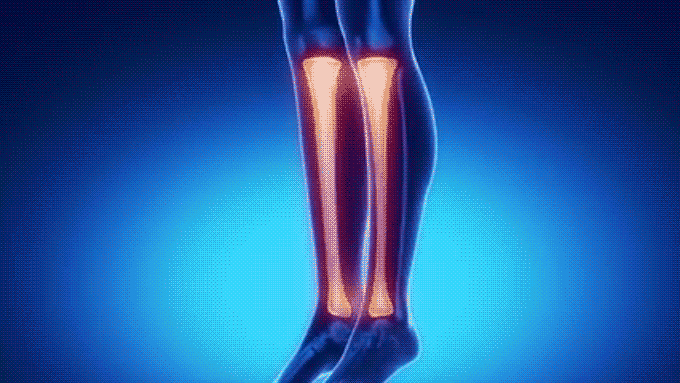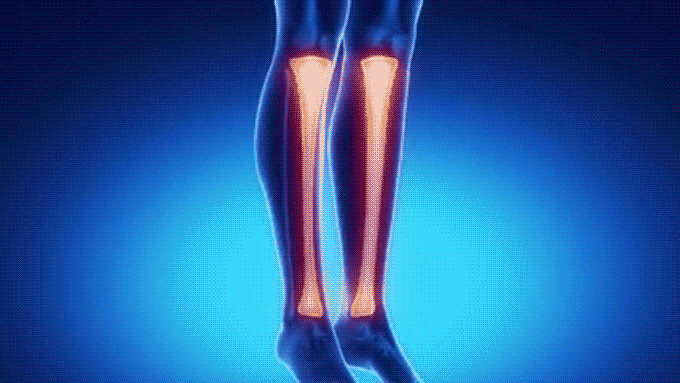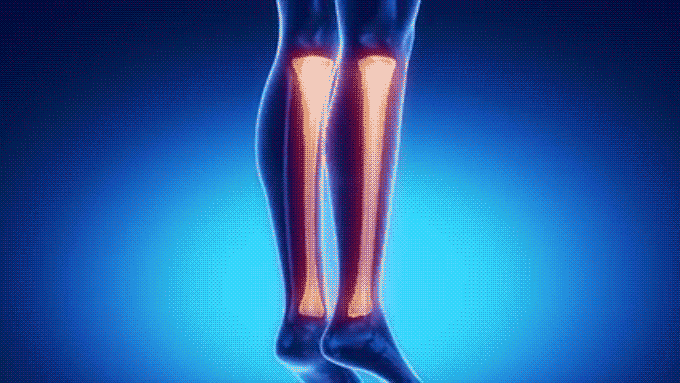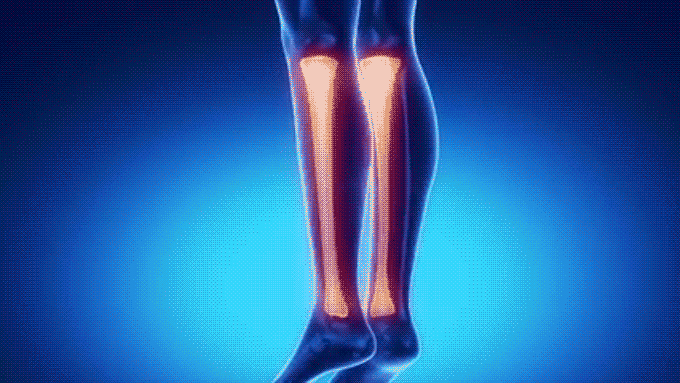
The tibia is one of two long bones in your lower leg that run between your knee and your foot. Also called the shinbone, the tibia is the larger and stronger of the two bones and carries more weight. Tibia fractures are common and usually caused by a sudden forceful injury, like a fall or motor vehicle accident. If the tibia fracture is severe, you may need surgery. Specific treatment will vary based on the type and severity of your fracture, but most people can be treated with an immobilizing cast and a strict regimen of non-weight bearing activity.
I
WHAT IS A TIBIA FRACTURE?
A tibia fracture is a break in the tibia bone, which is one of two long bones that make up your lower leg (the other is the fibula). The tibia is the larger and stronger of the two bones and has an important role to play because it supports most of your weight. Of all the long bones in the body – which include the upper leg femur, upper arm humerus, tibia and fibula – the tibia is the most commonly fractured. Around 4 percent of the senior population [1] experience a fractured tibia.
I
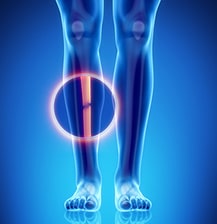
CAUSES AND TYPES OF TIBIA FRACTURES
Tibia fractures are usually caused by a sudden injury such as a fall, collision while playing sports, automobile accident or cycling accident. If the upper part of the bone is affected, it’s known as a proximal or tibial plateau fracture and if the lower part breaks, it’s called a distal or pilon fracture.
Due to the shape of the tibia, there are several different ways to fracture your tibia that include:

Stable (non-displaced) fracture
Most of the bone is left intact in its normal position. The bones stay in place during healing.
Displaced fracture
The bone no longer lines up properly. Surgery is usually needed to realign the bone and ensure correct healing.
Transverse fracture
The fracture is horizontal. It may still be stable depending on the location of the fracture and the stability of the fibula.
Oblique fracture
The fracture is diagonal or at an angle. While these oblique fractures can be initially stable, over time they can shift, resulting in the bones becoming displaced.
Spiral fracture
The fracture line resembles a spiral staircase, which is usually caused by a twisting movement.
Comminuted fracture
The bone breaks into several small pieces. It is inherently very unstable and is usually the result of a high-impact trauma, like a car accident.
Open fracture
Also known as a compound fracture, the break to the tibia is so severe that the bone has torn through the soft tissues and punctured the skin.
Stress fracture shin
A stress fracture of the shin is a small crack in the tibia caused by overuse. Symptoms usually occur slowly over time and are associated with a sudden increase in running or jumping. Treatment generally involves a regimen of rest, ice, compression and elevation (RICE) to allow the bone to heal, but stress fractures can be complicated injuries that require advanced levels of care. The first step in treating a stress fracture of the shin should be a visit to your doctor.
I
WHAT ARE COMMON SYMPTOMS OF A BROKEN TIBIA?
The main symptoms of a fractured tibia are:
- Immediate and severe pain,
- An inability to walk or put any weight on your injured leg,
- Bruising and swelling,
- Your leg may be an odd shape,
- Bone may be protruding through the skin,
- Some people feel faint, dizzy, or sick.
It you suspect you have a broken tibia, it’s important to seek medical help as soon as possible. In the meantime, put a cushion or pile of clothes underneath your leg for support and try not to move. Don’t try to walk on your injured leg because even simple movements could make the break worse and cause further problems, such as soft tissue damage.
Your doctor will examine your leg and ask questions about how the injury happened. If they suspect a broken tibia, they’ll order an X-ray or CT scan, a more sensitive imaging test, in order to see the bone in more detail.
I
TREATMENT OPTIONS FOR A BROKEN TIBIA
Treatment for a broken tibia depends on the type and severity of the injury. If the broken bone is stable, you probably won’t need surgery, but will need to wear a cast, splint or brace to hold the bone in place while it heals. As the bone heals your doctor may order a boot that provides support as your leg slowly heals and you start to bear weight.
A broken bone can cause a lot of swelling. If your leg is too swollen for a cast, you’ll be given a splint to wear instead. This will immobilize and support your leg, and it can be adjusted as your swelling goes down. Once the swelling has reduced enough, which can take anywhere from days to weeks, your doctor will decide if you need a cast, boot or surgery.
A broken tibia can be very painful. Over-the-counter medication can help manage the pain but if your symptoms are severe, your doctor may prescribe painkillers.

Tibia Fracture Surgery
If your fracture is unstable, displaced or angulated you’ll probably need surgery. There are several different surgical options to treat tibia fractures with different fixation techniques for each fracture pattern. These surgeries are usually performed under general anesthetic.
Surgeons will consider the location, type, and severity of the tibia fractures when deciding which method to use.
Intramedullary nailing (IMN): This technique involves inserting a specially designed metal rod from the front of your knee down the canal of the tibia. The rod passes across the fracture to keep it in position and is screwed to the bone at both ends. This procedure is popular because it keeps the bone aligned and allows for strong, stable fixation.
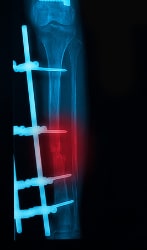
Open reduction internal fixation (ORIF): ORIF is sometimes referred to as “plates and screws.” It’s a method that can be used if nailing isn’t possible – usually when the fracture extends into the knee or ankle. During an ORIF tibia surgery, your surgeon will reposition bone fragments to their normal alignment and hold them together with special screws and metal plates that attach to the outer surface of the bone. Your surgeon probably won’t remove them unless they cause a problem.
External fixation: This procedure involves placing metal pins into the bone above and below the fracture. Your surgeon will position a bar outside the skin and attach it to pins that stabilize the frame and hold the bone in position. When the tibia is healed, the frame will be removed. External fixation is predominantly used to treat severe, open fractures.
I
HOW LONG DOES IT TAKE FOR A TIBIA FRACTURE TO HEAL?
Recovery time for a fractured tibia varies depending on the fracture pattern and type of treatment your surgeon uses. Most fractures heal completely in three to six months.
Wearing a Cast, Boot or Splint
Most patients initially wear a splint or half cast as the initial swelling subsides. Most patients then transition to a cast to hold the break in place while the bone heals.
Keep your leg elevated at the level of your heart, which will help reduce pain and swelling. You may find the cast feels itchy at first, but as tempting as it is don’t stick anything in the splint to scratch because even small abrasions can cause irritation or infections.
Splints and casts should be kept clean and dry, so you’ll need to protect them with a specialized cast bag when you shower. Some people use a plastic bag tied tightly around the cast. Be cautious because either method can leak.
Once your cast is removed, you may be given a special walking boot that will support your leg as you slowly begin to bear weight again. Your health professional will show you how to adjust the boot so that it fits correctly. The benefit of the boot is that it can be removed when you are resting and washing. Each physician will have specific instructions on how much to wear the boot and how much weight to place on the foot. Always follow your physician’s instructions.
Physical Therapy for a Fractured Tibia
Physical therapy can play an important role in your recovery from a fractured tibia. Your physical therapist may prescribe gentle exercises during the initial non-weight bearing phase to help reduce stiffness, strengthen the surrounding muscles, and prevent atrophy.
Once your physician allows you to start bearing weight again, your physical therapist will initiate exercises to build up strength and regain balance control. Muscle atrophies or shrinks shortly after an injury and even following a very brief period of non-weight bearing activity. Thus, restoring normal muscle function is paramount to returning to normal walking and daily activities.
I
CAN YOU WALK WITH A FRACTURED TIBIA?
Unless you have a minor stress fracture, your physician will likely ask you to stay off your injured leg completely for your initial phase of recovery. This non-weight bearing period is an extremely frustrating but necessary part of the recovery process. Any attempt to put weight on your injured leg before it’s ready, however, could prevent the bone from healing and may make the injury worse.
In order to comply with this important recovery phase, you’ll need to use a mobility aid such as crutches, a wheelchair, knee scooter, or the iWALK hands-free crutch.
Traditional Crutches
Traditional crutches are easy to find and inexpensive making them the first thing people usually try after surgery. However, crutches can be exhausting and cause pain in the underarms, forearms and wrists. They also restrict numerous day-to-day activities because you can’t carry anything, meaning activities like showering, grooming and eating are more challenging. Most patients find crutches so uncomfortable, however, that they cheat during the non-weight bearing phase of their recovery and walk on the injured leg before it’s healed. This can cause additional injury or slow the recovery.

Knee Scooters or Knee Walkers
Knee scooters, also referred to as knee walkers, are more efficient than crutches and require less upper body strength. They enable users to scoot easily from point A to point B without getting exhausted as long as they’re being used on flat surfaces. Their overall use is fairly limited, however, because they don’t work on stairs, slopes or uneven terrain. They also require use of your hands, so you can’t carry things. Finally, they are bulky which makes them difficult to transport.
Because knee scooters require you to rest your lower leg on a padded platform, they may not work for tibia fractures that occur in the upper part of the lower leg.

iWALK Hands-Free Crutch
The iWALK hands-free crutch facilitates unaided walking with full use of your hands and arms. It functions like a temporary lower leg so you can go about daily life while your injured leg remains safely and securely elevated. You can use the iWALK on stairs, slopes, uneven terrain and in the shower, and it makes everyday tasks like cooking, cleaning and carrying things around the house a breeze.
A 2019 medical study [2] found that nine out of 10 patients prefer the iWALK to traditional crutches. They reported less pain, less exhaustion, and less shortness of breath while using the iWALK. Another recent study [3] found that the iWALK simulates normal walking in a way that engages upper and lower leg muscles while immobilizing the lower leg and foot. This boosts blood flow in the immobilized extremity, which speeds recovery time. Engaging lower leg muscles while using the iWALK also avoids muscle atrophy that’s unavoidable using traditional crutches or knee scooters.
As with knee scooters, the iWALK requires you to rest your lower leg on a padded platform and may not work for fibula fractures that occur in the upper part of the lower leg.

I
FAQ
Do you need crutches for a stress fracture?
In most cases, the answer is no. Walking after a tibia fracture can make your injury worse and may cause further damage to the surrounding muscles, ligaments and skin. Walking on a fractured tibia is also likely to be extremely painful. If you suspect you might have broken your leg, don’t walk on it until you’ve seen a doctor. If you do have a broken tibia, you’ll probably need to be non-weight bearing which means you’ll need crutches, a wheelchair, mobility scooter, or hands-free crutch to get around. However, if you only have a minor stress fracture you may still be able to walk. Always consult with your doctor or surgeon before walking on a tibia fracture.
How long does it take for a tibia fracture to heal?
In most cases, the recovery time for a fractured tibia is six to 10 weeks, but recovery time will vary considerably depending on the patient and severity of the fracture. You may experience swelling for up to a year afterward. Minor stress fractures may take less time, and severe breaks may take more.
Can a tibia fracture heal on its own?
A fractured tibia doesn’t always require surgery, but it won’t heal properly on its own, either. Leaving it to heal on its own is risky and can leave the leg angulated and in chronic pain. A physician should treat and supervise a fractured tibia, and they will probably prescribe immobilization with a cast, splint or special boot and not putting any weight on it to ensure proper healing.
How long do you wear a cast for a broken tibia?
The length of time you need to wear a cast for a broken tibia depends on how severe your injury is, but it will likely be at least six weeks. Your doctor will probably prescribe use of a walking boot for a few additional weeks. The boot will support your leg as you slowly start to bear weight again.
How do you help someone with a broken leg?
If you suspect someone has broken their leg, seek medical help as soon as possible. If they’re unable to get to the Emergency Room, you may need to call an ambulance.
The information above is intended for informational purposes only and is not intended to prevent, treat, or diagnose any illness or disease. We aim to provide the highest quality information, so if you have any questions on the information above, we welcome your feedback!
- Thompson JH, Koutsogiannis P, Jahangir A. Tibia Fractures Overview. [Updated 2021 Aug 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan. https://www.ncbi.nlm.nih.gov/books/NBK513267/
- Martin KD, Unangst AM, Huh J, Chisholm J. Patient Preference and Physical Demand for Hands-Free Single Crutch vs Standard Axillary Crutches in Foot and Ankle Patients. Foot & Ankle International. 2019. https://journals.sagepub.com/doi/abs/10.1177/1071100719862743
- Dewar C, Martin KD. Comparison of Lower Extremity EMG Muscle Testing With Hands-Free Single Crutch vs Standard Axillary Crutches. Foot & Ankle Orthopaedics. July 2020. 3. https://journals.sagepub.com/doi/full/10.1177/2473011420939875
- Jason A. Low, M.D. Tibia (Shinbone) Shaft Fractures. OrthoInfo. May 2018. https://orthoinfo.aaos.org/en/diseases–conditions/tibia-shinbone-shaft-fractures
- Mike Walden. Tibia Fracture. SportsInjuryClinic. 15 April 2021. https://www.sportsinjuryclinic.net/sport-injuries/lower-leg/shin-pain/tibia-fracture
- Tibia Plateau Fracture. Arlington Orthopedics Association. https://www.arlingtonortho.com/conditions/knee/knee-tibial-plateau-fracture/
The Best Mobility Device
for Tibia Fractures.
The Best Mobility Device
for Tibia Fractures.
Free 1-2 Day Delivery
to most locations


