Lower Leg Injury Resource Center
Stress Fractures
Causes and Key Treatment Options
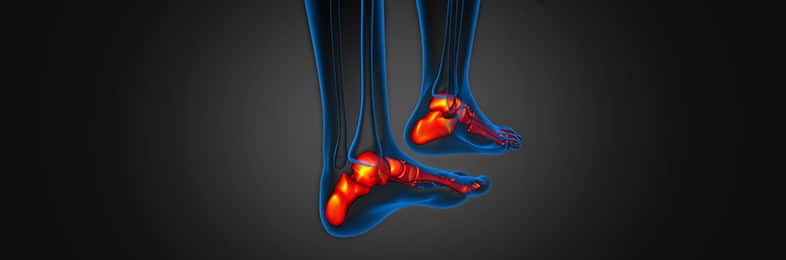
Stress fractures are breaks in bones caused by repeated force on a bone and can range from very mild to quite severe (1). Stress fractures are difficult to self-diagnose because the symptoms (pain and swelling) are similar to other types of injuries. The following article will describe the features and causes of stress fractures in the lower leg and will discuss common treatments, therapies, and recovery.
I
WHAT IS A STRESS FRACTURE?
A stress fracture, also known as a hairline fracture, is a small break in a bone. It is more common in the weight bearing bones of the lower leg and foot – 73% of stress fractures occur in this area of the body (1).
It’s usually caused by overuse and is a common sporting injury, especially in athletes who do a lot of running or jumping. It is also known to affect military recruits – the injury was first identified in the 1850s by a Prussian army physician who frequently saw it happen to soldiers when taking part in heavy training and long road marches.
A stress fracture can also develop from normal, everyday use of a bone that’s been weakened by age or a condition like osteoporosis.

Stress fractures can range in severity. You may only notice a dull pain that comes and goes at first. However, a severe fracture or a fracture left untreated can become increasingly painful, preventing you from walking or even standing without support.
I
CAUSES OF STRESS FRACTURES
A stress fracture is caused by overuse and is common among recreational and professional athletes, especially those who do high-impact sports like track and field, dancing, basketball, tennis, or gymnastics. Stress fractures account for up to 20% of athletic injuries (2) and can affect people of all fitness levels.
There are some other factors which can cause or increase the chance of developing a stress fracture:
Bone insufficiency
Medical conditions such as osteoporosis and certain medications, like heparin and warfarin, can lower bone density and make your bones more susceptible to becoming overloaded by even minor stresses, resulting in a stress fracture.
Insufficient conditioning
Stress fractures often occur when bones are subjected to a new activity and have some trouble adjusting. This can happen to athletes of all levels when they start a new type of activity or quickly return to an exercise regime after a period of rest.
Poor technique
Having the correct technique while exercising is important to minimize injuries like stress fractures. Poor technique can be down to lack of experience or training, or because of another condition like a blister or bunion which affects the way your foot hits the ground or causes you to favor one leg over another.
Improper equipment
Using proper equipment is really important when exercising. This could be as simple as having well-fitting trainers that provide enough padding to absorb the shock and stresses of high-impact sports.
Gender
Women are more likely to get stress fractures. This is thought to be a result of several factors such as infrequent menstrual cycle, low body mass index, low energy intake, and sometimes low bone mass.
I
PREVENTION OF STRESS FRACTURE
Stress fractures are not inevitable. They can be avoided by paying attention to things like proper technique, gear, and training schedules, as well as by maintaining a healthy diet and varying your physical activities (7). Perhaps most importantly, pay attention to your body. Take a break from any activity that causes repeated pain. If a few days of rest doesn’t relieve your pain, contact your physician for a more in-depth examination.
Most stress fractures don’t require surgery. Instead, a pain reliever is likely to be prescribed, and the patient will be directed to rest and refrain from putting weight on the fractured limb. Commonly prescribed pain medications include ibuprofen (trade names: Motrin, Advil, Nupirn) or naproxen (trade names: Aleve, Midol, Naprosyn). If the injury is mild and some weight can be put on the limb, the physician may prescribe a walking boot or brace. These stiff, bulky devices allow a person to walk hands-free with only minor disruptions to normal walking gait (8).
For more severe stress fractures, the physician will direct the patient to be non-weight bearing. No weight should be put on the injured limb for the recommended time frame (generally 1 to 3 weeks for a stress fracture), and the prescription tends to consist of a combination of bed rest, an assistive device, and physical therapy (9). When a person is prescribed non-weight bearing, crutches tend to be the first device that comes to mind. Fortunately, there are new advances in non-weight bearing medical technology, which allow non-weight bearing activity with additional mobility. Because it is so important to follow the non-weight bearing prescription, it is necessary to figure out which device will work best for you. The various options are explained below.
I
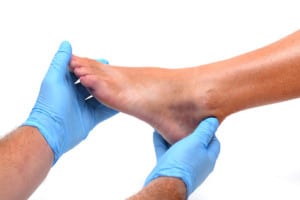
STRESS FRACTURE SYMPTOMS AND DIAGNOSIS
Stress fractures typically start as a dull pain, localized to the site of the injury. You may notice some swelling too. You may only feel pain when doing certain activities and find that it decreases or goes away when you stop. However, over time the pain can become more persistent and start to affect your daily life.
Stress fractures can be hard to diagnose because the symptoms are similar to other injuries, like bruising of the bone, shin splints, strains, sprains and plantar fasciitis. If you’re experiencing pain during exercise, speak to your doctor. It’s important to get checked out because a small fracture left untreated will probably get worse.
Your doctor will examine your injury and ask you how long you’ve been experiencing pain, what makes it better or worse, and if it has changed over time. If they suspect a stress fracture, they will order an MRI or CT scan to confirm the diagnosis. These types of imaging tests tend to be more effective because tiny breaks are difficult to detect in the early stages and may not get picked up in an X-ray.

I
TREATMENT OPTIONS FOR STRESS FRACTURE
Most stress fractures don’t require surgery. You will probably be prescribed rest and pain relief and told to apply ice to reduce any swelling or discomfort. Commonly prescribed pain medications include ibuprofen or naproxen. You may also be given a protective walking boot or brace to wear.
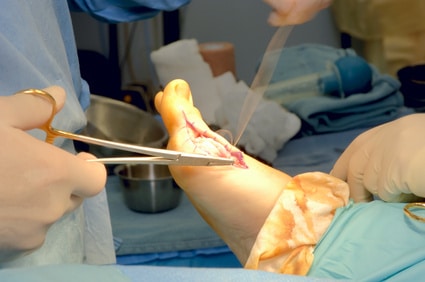
If the bone doesn’t heal correctly with non-surgical treatment, surgery may be required. This typically involves either using screws to secure the bone or grafting new bone into the space that the fracture has left open.
The amount and level of rest you need to recover will depend on your injury. It can vary from simply avoiding the exercise that causes pain to not putting any weight on your leg at all. Make sure that you stick to the treatment plan your doctor gives you otherwise it may prevent the injury from healing or lead to the bone healing out of alignment. Any pain or swelling should subside with proper recovery and rehabilitation.
I
STRESS FRACTURE RECOVERY AND REHABILITATION
It usually takes six to eight weeks for a stress fracture to heal completely. While you recover you’ll need to rest and avoid any activity which causes pain. For more severe stress fractures, you may need to be completely non-weight bearing. This means that you can’t put any weight on your injured limb at all, usually for one to three weeks. This can be frustrating but it’s important to stick to the rules in order to make a full recovery.
Once your doctor gives you the green light, you’ll slowly be able to resume normal activities again. Physical therapy can condition and strengthen your muscles, helping them to absorb the stress of activities and possibly reduce the risk of reoccurrence.
If your doctor prescribes a period of non-weight bearing you may be given crutches, which can be very restrictive. Fortunately there are new advances in non-weight bearing medical technology which allow you to stay active while you recover.

Below are your main mobility options:
Traditional Crutches
Crutches are the best-known mobility aid for people recovering from lower leg injuries. They are relatively cheap and easy to get hold of but they have limitations. Firstly, you lose the use of your hands and arms as well as your leg, making simple tasks like carrying a cup of coffee impossible. They are pretty exhausting, leaving you feeling like you’ve climbed a mountain simply after going up some stairs. Crutches can also cause additional pain in your hands, arms and back.

Knee Scooters or Knee Walkers
Knee scooters or knee walkers are a good alternative to crutches because they enable you to move around freely while keeping your injured leg elevated. They also require less upper body strength than crutches so they’re not as exhausting to use.
However, they can’t be used on stairs, slopes, or uneven terrain. They also require the use of both arms to navigate the scooter which, like crutches, can be restrictive.

iWALK Hands-Free Crutch
The iWALK hands-free crutch is now a popular option because, unlike the other devices, it’s completely hands-free. It functions like a hi-tech peg-leg so you can walk around freely and unaided while your injured limb remains elevated. You can use the device on stairs, slopes, uneven ground, and even in the shower. A 2019 medical study (3) found that nine out of ten patients prefer this device to traditional crutches.

Despite being painful and inconvenient, stress fractures are frequently mild injuries that can be treated non-surgically. Generally, a combination of pain medication, rest and a non-weight bearing device enabling movement without putting weight on the injured limb are all that is needed to reach full recovery. Remember, if prescribed a non-weight bearing period, it is very important to choose the medical device that will work best for your lifestyle. Initial medical treatment should be followed by physical therapy, to enable timely recovery and avoidance of future stress fractures.
I
FAQS
Here are some of the most frequently asked questions about stress fractures:
Do you need crutches for a stress fracture?
It depends. If your stress fracture is mild, your doctor may simply tell you to rest it regularly and refrain from doing any activity that causes pain. However, for more severe stress fractures, you might need to be non-weight bearing for a while, usually between one to three weeks. During this time you’ll need to use conventional crutches or an alternative, like a knee scooter or the iWALK hands-free crutch.
Can you walk with a stress fracture in the foot?
Your doctor will advise you about whether it’s okay to walk if you have a stress fracture. You may be given the green light to carry on with daily activities and just avoid high-impact sports. However, if your injury is more severe, you may need to be non-weight bearing for a few weeks so that it can properly heal.
Can you prevent stress fractures?
You can’t protect yourself from stress fractures completely but there are some things that you can do to reduce the risk. Pay attention to your technique and make sure that you’re using high-quality exercise equipment and wearing proper, well-fitting running shoes. Ease yourself into any new or modified fitness regime slowly and build up gradually, making sure you get enough rest in between sessions.
Pay attention to your body and take a break from any activity that is causing repeated pain. Lower impact sports like swimming and cycling can help to take the pressure off your weight-bearing bones while enabling you to stay active. If a few days of rest don’t relieve the pain, go and see your doctor.
Can you have a stress fracture and not know it?
Yes. The pain can feel mild at first and only occur during certain types of exercise, so you may think it’s just a niggle which will go away on its own. It’s only when the pain becomes persistent that many people realise it might be something more serious.
What happens if a fracture is left untreated?
A stress fracture left untreated will most likely worsen and become increasingly painful. It can lead to long term problems and eventually the bone may break completely.
How painful is a stress fracture?
If it’s mild it may not feel that painful at all. You may only notice a dull pain when exercising which stops when you rest. But if left untreated, the pain will most likely worsen over time and become more persistent.
What is the fastest way to heal a stress fracture?
There’s no quick fix for a stress fracture unfortunately – it will improve with rest and time. The most important thing is to see your doctor so that you can determine how severe your injury is and what treatment you need in order to make a full recovery.
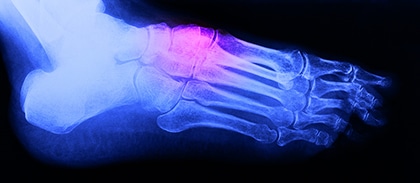
Do stress fractures show up on an X-ray?
Stress fractures don’t always show up on X-rays in the early stages as they’re too small, so your doctor will probably suggest an MRI or CT scan to confirm the diagnosis instead. These imaging tests are more sensitive and can spot hairline fractures.
The information above is intended for informational purposes only and is not intended to prevent, treat, or diagnose any illness or disease. We aim to provide the highest quality information, so if you have any questions on the information above, we welcome your feedback!
- https://www.aafp.org/afp/2011/0101/p39.pdf
- https://academic.oup.com/jcem/article/102/2/525/2972072
- https://www.ncbi.nlm.nih.gov/pubmed/31375043
The Best Mobility Device
for Stress Fractures.
The Best Mobility Device
for Stress Fractures.
Free 1-2 Day Delivery
to most locations


