Lower Leg Injury Resource Center
Charcot Foot
Causes, Diagnosis and Treatment
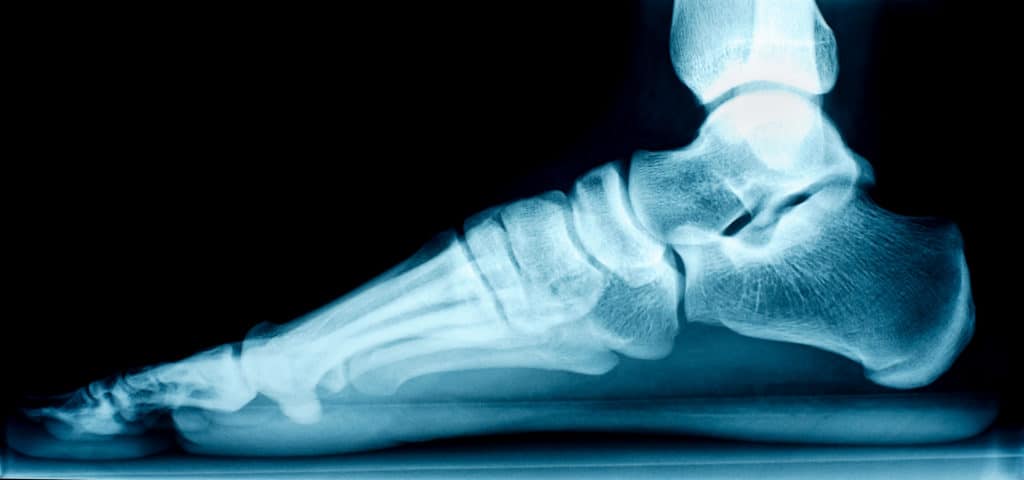
Charcot foot is a rare but serious disease that impacts the bones, nerves and tissue in your feet. The condition affects people with nerve damage, usually as a result of diabetes, and this underlying nerve damage, called neuropathy, makes it difficult for people to know their feet are injured. Over time, this can lead to fractures, sprains or sores that change the shape of the foot.
If you’re at risk, it’s important to take steps to prevent Charcot foot, and you should seek medical help as soon as possible if you notice symptoms.
I
WHAT IS CHARCOT FOOT?
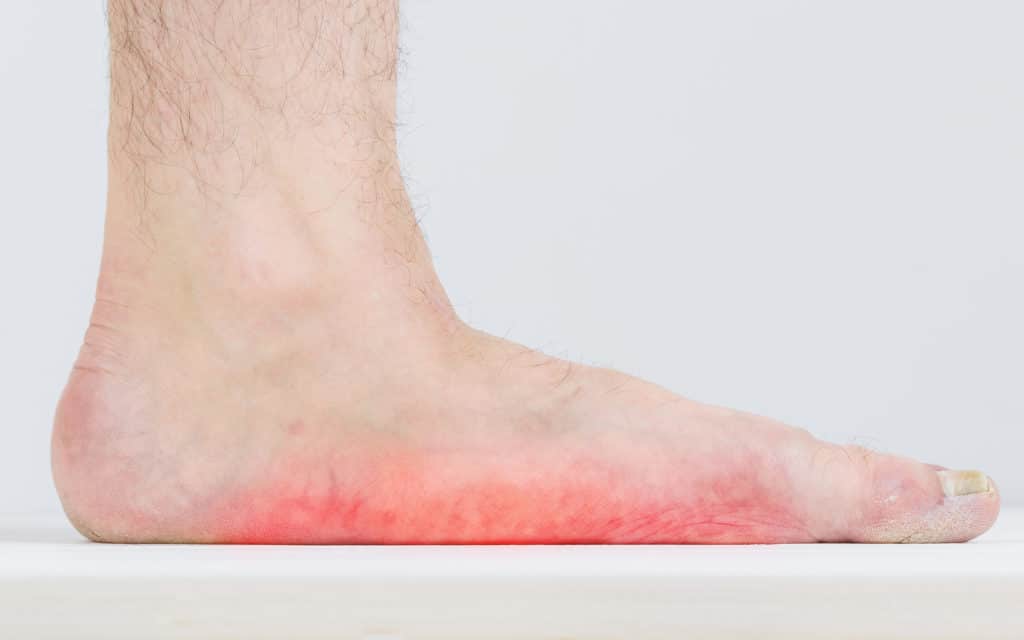
Charcot foot is a condition where the bones in your feet become very fragile. This makes them susceptible to breaking or dislocating, even from minor forces that come from everyday activities like standing or walking. Over time, the joints can collapse and the foot can change shape, leading to permanent deformity and disability. Medical terms for the condition are Charcot arthropathy and Charcot neuroarthropathy.
I
WHAT CAUSES CHARCOT FOOT?
Charcot foot affects people who have significant nerve damage, called peripheral neuropathy. This is usually a complication of diabetes, but other factors can cause it including alcohol or drug abuse, syphilis, an infection, spinal disease or spinal injury, HIV, or Parkinson’s. It’s a rare condition that affects about 1 percent of people with diabetes [1]. It usually develops in one foot, but in some people both feet can be affected.
Many patients with Charcot foot have had poorly controlled diabetes for 15 to 20 years [2]. There is also often an injury that triggers the condition, like a foot or ankle injury, an infection that doesn’t go away or sore that doesn’t heal.
Neuropathy causes loss of feeling, which means people experiencing a recent injury may not realize they’ve hurt themselves and continue to stand and walk. This can make the injury worse and lead to foot bones becoming dislocated or fractured.
As bones weaken, the joints can collapse, and this changes the shape of your foot. Depending on the location of the bone break, the arch of your foot may collapse and cause a rocker bottom foot. Your toes may start to curve under your foot, or your ankle may become unstable.
Charcot foot can also cause foot sores and infection. If left untreated, the condition can lead to permanent deformity, disability and, in some cases, amputation.
I
SYMPTOMS AND DIAGNOSIS OF CHARCOT FOOT
Charcot foot can be difficult to diagnose at first, so it may go unnoticed for a period of time. A common early sign is inflammation in your foot or ankle. This can cause swelling, heat and redness. You may experience some aching or discomfort, but for many people it is painless because of the underlying nerve damage.
If you continue to walk with the condition you may begin to notice your foot changing shape and becoming deformed. The longer Charcot foot goes undetected the harder it is to treat. If you have neuropathy, and foot or ankle issues are bugging you, it’s important to seek medical attention as soon as possible, no matter how minor you think these issues are.
Diagnosing Charcot Foot
If you’re at risk and have symptoms, you should visit a specialist experienced at diagnosing Charcot foot. The doctor will examine your foot for changes in appearance and may carry out some painless tests, such as temperature testing of the skin to see if your suspect foot has increased in temperature, a common symptom of the condition. You may be asked to stand and walk so your doctor can study your weight distribution. They will ask about your medical background and when you first noticed symptoms.
X-rays will help your doctor to examine the bones and joints in your feet. If your doctor needs more information to make a diagnosis, they may order an MRI, which is a more sensitive imaging test that can detect small bone fractures and inflammation, both early signs of Charcot foot.
I
WHAT IS THE BEST TREATMENT FOR CHARCOT FOOT?
Charcot foot needs to be treated as soon as possible. Any delay may make the deformity in your foot much worse. Treatment involves reducing pressure on your foot and wearing a cast to allow the bones, ligaments and tendons of your foot to rest, set and heal.
It can take several months to treat Charcot foot. Your doctor may prescribe a cast or walking brace for up to eight months. This will immobilize your foot and help prevent further injury. During this time, you will be completely or partially non-weight bearing, which means not putting weight on your foot. You’ll need to use a mobility device like crutches, a wheelchair, knee scooter or hands-free crutch to get around.
Once your doctor gives you the go-ahead, you’ll be able to stand on your foot again with the help of special shoes and orthotics that offer your foot additional support. Your doctor may also advise that you modify your activities to avoid repetitive trauma to your feet.
Charcot Foot Surgery
If your condition is severe, your doctor may choose to repair the bones through surgery. During the operation, they will realign or fuse bones to make your foot more stable. They may also smooth sharp bones that could cut into your skin and cause sores.
Studies have shown good outcomes for people who have surgery to treat Charcot foot. Nearly four out of five diabetic patients [3] with severe cases were able to walk normally again after surgery.
Amputation for Charcot Foot
In severe cases, Charcot foot may require amputation. This is usually the result of ulcers and infections that develop because of foot deformity. Studies have found that 2.7 percent of people [4] with Charcot foot will need to have amputation.
The condition should be diagnosed and treated as soon as possible to avoid the chance of developing ulcers, which increases the likelihood of amputation.
I
RECOVERY FROM CHARCOT FOOT
The length of time it takes to recover from Charcot foot varies based on the severity of the condition, but it can take many months. Regular check-ups with a specialist will be required to monitor progress.
You may need to wear a cast for up to eight months. This can be a frustrating experience, but it’s essential not to cheat and put weight on your foot, which could delay your recovery and cause further problems.
During this period, you’ll need to use a mobility device to help you get around, and there are a number of options.
Wheelchairs
Wheelchairs can be a good option for people with Charcot foot in both feet or who are unable to use other devices for physical reasons. There are manual and powered wheelchairs. Manual chairs require more upper body strength and can strain your back, shoulders and neck. Power wheelchairs make it easier to move around without effort.
If you can use them, other mobility devices will help you stay active during your recovery, and that can have a huge effect on your physical and mental health.

Traditional Crutches
Traditional crutches are easy to find and inexpensive, but they can be tiring to use and can cause pain in your arms, wrists and hands. Crutches are also restrictive because you can’t carry anything, which prevents you from performing normal day-to-day activities. Crutches generally decrease patients’ motivation to comply with the non-weight bearing phase of their recovery, and that can cause additional complications.

Knee Scooters or Knee Walkers
Knee scooters, also called knee walkers, are more efficient than crutches and require less upper body strength. They are excellent on flat surfaces and make it possible to scoot from one place to another without getting exhausted. They don’t, however, work on stairs, slopes or uneven terrain. Knee scooters also require use your hands to steer and balance, so you can’t carry things while using them. Finally, knee scooters are bulky, which makes them difficult to transport. It’s also challenging to navigate tight environments using a knee scooter.

iWALK Hands-Free Crutch
The iWALK hands-free crutch enables you to walk around unaided with full use of your hands and arms. It functions like a temporary lower leg, so you can go about your daily life while your injured foot remains safely and securely elevated. It can be used on stairs, slopes, uneven terrain and in the shower.
A 2019 medical study [5] found that nine out of 10 patients prefer the iWALK hands-free crutch to traditional crutches. Another recent study found that using the iWALK increases blood flow, reduces muscle atrophy and may speed recovery. This quick test can help you decide if the hands-free crutch is a good option for you.

I
CAN I PREVENT CHARCOT FOOT?
You can’t entirely prevent Charcot foot, but there are a number of actions you can take to help reduce the risk.
- Keep your blood glucose level under control.
- Check your feet every day for signs of damage or injury.
- Be careful to avoid injury.
- Have regular check-ups with a foot and ankle specialist.
I
CHARCOT FOOT FAQ
Here are the most commonly asked questions about Charcot Foot:
Is Charcot foot permanent?
If Charcot foot is detected and treated quickly, it can heal with time. However, if your foot has already changed shape due to fractures, sprains and development of sores, this is permanent and can’t be reversed. The condition may return, but the correct treatment will help reduce chances of this happening.
Is Charcot foot painful?
Patients who develop Charcot foot have neuropathy, which causes loss of feeling. This means many people don’t feel any pain at all, which is why the condition can worsen before it’s detected. Some people have reported feeling pain and soreness in their foot.
Can you walk with Charcot foot?
Many people continue to walk with Charcot foot because they don’t realize they have an injury. Once the condition has been diagnosed, you must stop weighting the injured foot to give your bones a chance to heal. Your doctor will prescribe a treatment plan. It’s essential that you stick to this plan because any attempt to walk sooner than prescribed can prevent recovery and may make the condition worse.
Is Charcot foot rare?
Charcot foot is very rare and develops in people with nerve damage, usually as a result of diabetes. Around 1 percent of people with diabetes are thought to develop the condition.
Can you have Charcot foot without diabetes?
Charcot foot affects people with nerve damage. The most common cause is diabetes, but other causes may include alcohol or drug abuse, syphilis, an infection, spinal disease or spinal injury, HIV or Parkinson’s.
The information above is intended for informational purposes only and is not intended to prevent, treat, or diagnose any illness or disease. We aim to provide the highest quality information, so if you have any questions on the information above, we welcome your feedback!
- Sohail Yousaf, Edward J.C. Dawe, Alan Saleh, Ian R. Gill, Alex Wee. The acute Charcot foot in diabetics. EFORT Open Reviews Vol. 3, No. 10. 24 Oct 2018. https://doi.org/10.1302/2058-5241.3.180003
- Todd C. Sommer, D.O., D.P.M., Thomas H. Lee, M.D. Charcot Foot: The Diagnostic Dilemma. American Family Physician. 1 November, 2001. https://www.aafp.org/afp/2001/1101/p1591.html
- Michael S Pinzur, Adam P Schiff. Deformity and Clinical Outcomes Following Operative Correction of Charcot Foot: A New Classification With Implications for Treatment. March 2018. National Library of Medicine. https://pubmed.ncbi.nlm.nih.gov/29172758/
- Charles L Saltzman, Mark L Hagy, Bridget Zimmerman, Miriam Estin, Reginald Cooper. How effective is intensive nonoperative initial treatment of patients with diabetes and Charcot arthropathy of the feet? National Library of Medicine. June 2005. https://pubmed.ncbi.nlm.nih.gov/15930937/
- Kevin D Martin, Alicia M Unangst, Jeannie Huh, Jamie Chisholm. Patient Preference and Physical Demand for Hands-Free Single Crutch vs Standard Axillary Crutches in Foot and Ankle Patients. National Library of Medicine. 2 August 2019. https://pubmed.ncbi.nlm.nih.gov/31375043/
The Best Mobility Device
for Charcot Foot.
The Best Mobility Device
for Charcot Foot.
Free 1-2 Day Delivery
to most locations


