Lower Leg Injury Resource Center
Bunions
Symptoms, Causes, Treatments, Surgery and Recovery
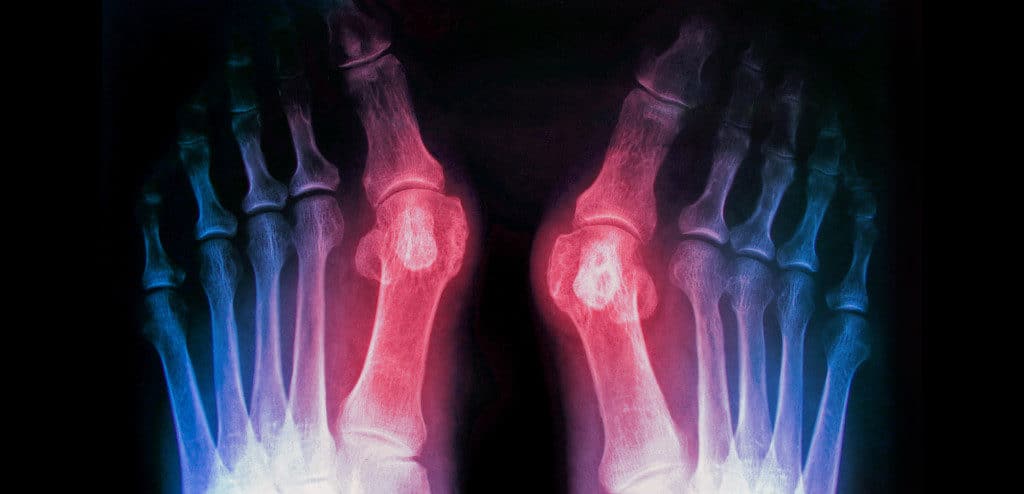
Bunions are bony lumps that form on the sides of your feet. They are very common, and most people learn to live with them by making lifestyle adjustments, such as wearing wider shoes. Bunions sometimes become sore and painful, however, and if they start to affect your daily life, surgery may be an option.
I
WHAT IS A BUNION?
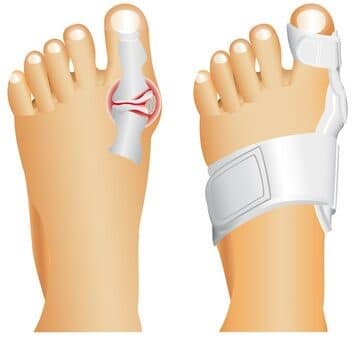
A bunion is a bony bump that develops on the inside of your foot at the base of your big toe. It’s an important joint that helps distribute body weight across your foot when you’re walking, running or standing.
Bunions form when bones at the front of your foot move out of place. This usually happens slowly, causing your big toe to move toward the smaller toes and forcing the joint at the base of your big toe to stick out. This condition, also known as hallux valgus, can gradually worsen over time and may become painful.
I
COMMON BUNION SYMPTOMS
Bunion symptoms can range from benign to painful. In general, look for one or more of the following symptoms.
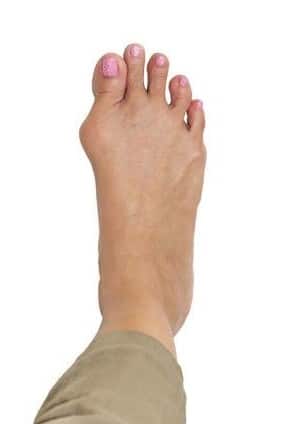
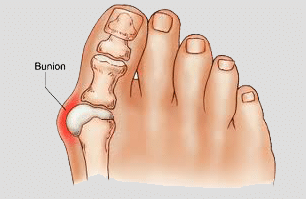
What does a bunion look like?
- Your big toe points toward your second toe, or your second toe overlaps your big toe.
- There’s a prominent bump on the inside of the big toe joint.
What does a bunion feel like?
- You experience pain on the inside of your foot at the big toe joint when wearing shoes.
- You experience pain when walking.
- There’s redness, swelling or thickening of the skin on the inside of the big toe joint.
I
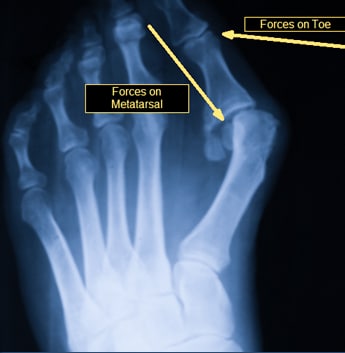
WHAT IS THE MAIN CAUSE OF BUNIONS
Bunions are a common condition and affect about one in three people over the age of 65 [1]. Women are more likely to be affected than men because they often wear tight, high-heeled shoes that squeeze toes together. While experts can’t agree on whether wearing tight shoes actually causes bunions in the first place, it’s clear that tight shoes make the problem worse. They’re less common in cultures where people don’t wear shoes at all.
While there’s a connection between footwear and bunions, the condition also often runs in the family. Your foot type, shape and underlying structure are hereditary and can affect your chances of getting bunions. If you have arthritis, weak connective tissue, a joint condition or short Achilles tendons or calf muscles, you’re also at a greater risk. The condition seems to develop faster in people who are flat-footed.
I
DIAGNOSING BUNIONS
Your doctor can usually diagnose bunions with a simple examination of your foot, but they may order an X-ray to get a clearer diagnosis. Your doctor will ask about your symptoms and watch you walk to understand your level of discomfort and its impact on your day-to-day life.
I
WHAT IS THE BEST TREATMENT FOR BUNIONS?
Most bunions only cause mild symptoms, and, while they won’t go away, non-surgical treatment can help manage or prevent the discomfort they’re causing. Sometimes, however, bunions will cause severe pain and pressure. If this pain affects your quality of life it may be time to discuss surgical options with your doctor.
Non-Surgical Bunion Treatment
Most people find relief from bunion pain by simply changing the types of shoes they wear. Get your feet measured to make sure you’re wearing the right size and choose comfortable, wider shoes that give your feet and toes ample room to move. If your big toe has plenty of space, it’s less likely to be pushed toward the smaller toes. Avoid heels higher than two inches because they usually put too much pressure on the front of your foot.
How to fit shoes for bunions:
- Size varies among shoe brands, so judge a shoe by how it fits rather than its marked size.
- Find a shoe that’s matches the shape of your foot.
- Measure your feet regularly. Foot size can change as you age.
- Many people’s feet are different sizes. Fit to the size of your largest foot.
- Stand during the fitting process.
- Be sure you can extend all of your toes and that there’s adequate space for your longest toe.
- Walk in the shoes to make sure they feel right.
Bunion cushions: You can also use pads or cushions that wrap your bunion and soften its contact with shoes. This can help relieve pain and prevent further growth.
Orthotics: Some doctors recommend using shoe inserts called orthotics, which ensure proper support and alignment of your foot. Especially when paired with a properly-fitting shoe, orthotics can reduce pressure on your bunion and help resolve or prevent other foot issues as well. Orthotics can be bought over the counter, but custom-made orthotics will provide the most tailored fit for your feet.
Bunion taping technique: Taping can reduce pressure on the inflamed joint and help your foot achieve proper alignment. Reach out to your doctor or physical therapist to learn the proper taping technique for your foot.
Anti-inflammatory techniques: Over-the-counter anti-inflammatory medications such as aspirin, ibuprofen or naproxen can help ease inflammation and pain. Applying ice can also help. Wrap a bag of frozen vegetables or ice in a towel and hold it over the area for about five minutes, making sure not to exceed 20 minutes to prevent skin damage.
Hot-Cold Bunion Therapy: Alternating ice with heat can also provide temporary pain relief and may also help reduce swelling or bursitis in the big toe joint.
Castor Oil: Castor Oil is an established anti-inflammatory and pain reliving holistic remedy that has been shown to relieve the discomfort caused by bunions. Wrap a castor oil soaked cloth around your foot and ensure the oil is in contact with the inflamed area. Wrap the entire foot with plastic wrap. Finally, place a hot compress for approximately 30 minutes.
Cortisone Injections: Inflammation of the joint at the base of the big toe and the pain associated with it can sometimes be relieved with a local injection of cortisone, a strong steroid used to reduce inflammation.
Acupuncture: This Chinese medical practice involving needles inserted at specified sites around the body has been shown to alleviate the pain caused by bunions.

Surgical Treatment for Bunions
If your bunion pain has become unmanageable it may be time to think about surgery. Surgery is the only way to permanently get rid of bunions.
Surgery is also the most drastic treatment and isn’t usually recommended just to improve the appearance of your feet. The procedure is called bunionectomy, and it typically involves removing the bony growth of the bunion and realigning the ligaments and tendons of the big toe joint.
An osteotomy to treat a bunion is a more invasive surgery that involves cutting and realigning the bone that forms the bunion. With this procedure, screws and pins are inserted into the bone to fix the realignment in place. Other types of bunion surgery include removing part of the bone in the big toe to straighten it or joining the bones of the joint permanently.
Bunion surgery is usually performed as an outpatient procedure, so you won’t need to stay in the hospital overnight. Surgery typically takes about an hour.
I
RECOVERY FROM BUNION SURGERY
Recovery from bunion surgery typically takes several weeks. Depending on the type of surgery you choose, you’ll wear either a cast, splint or orthopedic walking boot after your operation and have to prevent the wound from getting wet while showering or bathing.
You won’t be able to put weight on your affected foot for the first couple of weeks after surgery. If you push the timeline and weight your foot prematurely you could disrupt the newly reset alignment of your foot and make your condition worse.
Once you’ve got the go-ahead from your doctor, you can slowly start putting weight on your foot again, and a full recovery can take up to six months.
Mobility Options While Recovering from Bunion Surgery
Going through a period of non-weight bearing activity is often the toughest rule to follow after foot surgery. It can be frustrating to have difficulty fetching yourself a cup of coffee or feeling exhausted after using crutches just to cross a room. There are options, however, to traditional crutches that can ease you through your period of non-weight-bearing activity and help ensure that you don’t put weight on your recovering foot too early.
Traditional crutches
Traditional crutches are the most common mobility device used by patients recovering from lower leg and foot surgeries. They are relatively cheap, easy to obtain and lightweight to transport. However, they quickly become frustrating and exhausting. Crutches require the full attention of your arms and hands, which can become sore from the stress of carrying your bodyweight.
Knee Scooters or Knee Walkers
Knee scooters, also called knee walkers, can be a great alternative to crutches because they enable you to move around freely while keeping your foot elevated. You can whizz around on flat surfaces, but you can’t use knee scooters on uneven ground or stairs, and they’re bulky to get in and out of cars. In addition, your hands and arms are required to navigate with a knee scooter, making them unavailable for other common tasks.
iWALK hands-free crutch
The iWALK hands-free crutch is a popular option among patients recovering from bunion surgery. It functions like a hi-tech pirate leg and allows you to walk freely and unaided without putting weight on your recovering foot at all. The iWALK gives you full use of your hands and arms and works on stairs and uneven ground. A 2019 medical study found that nine out of 10 patients prefer the iWALK to traditional crutches [2]. Another recent study showed that the iWALK facilitates improved blood flow in your injured foot, limits muscle atrophy and may speed recovery.

I
BROKEN ANKLE FAQ
What is the difference between a bunion and hallux valgus?
Hallux valgus and bunions are the same condition. Hallux valgus is merely the medical term.
Do bunions ever go away on their own?
Bunions do not go away on their own. The only way to get rid of them is to have surgery.
Should I have bunion surgery?
Surgery is usually only recommended if your symptoms are severe and other treatments haven’t worked. Bunion surgery is not typically performed for cosmetic reasons. As with all surgeries, there are risks. In a medical study of patients who had bunion surgery, 82 percent were either very pleased or fairly pleased with the outcome eight years later [3].
Is bunion surgery painful?
Most people will experience some pain and discomfort for the first few days after bunion surgery. Your medical team will offer advice about how to minimize pain and swelling. The long-term aim of surgery is to eliminate the pain caused by your bunion.
Do bunions get worse as you age?
Many bunions are progressive and will worsen over time. Studies have found that the prevalence increases with age, particularly in women [4].
What exercises help bunions?
Foot exercises won’t get rid of bunions, but they can help relieve some of the symptoms. Common exercises include:
- Stretching your toes: Point your toes straight ahead for five seconds and then curl them under for five seconds. Repeat 10 times.
- Toe circles: While sitting, hold your big toe and circle it clockwise a few times. Then do the same anticlockwise. Repeat several times.
- Ball rolls: Put a small ball like a tennis or golf ball under your foot and roll it around for a few minutes.
- Towel curls: Put a small towel on the floor, grip it with your toes and pull it toward you. Repeat several times.
The information above is intended for informational purposes only and is not intended to prevent, treat, or diagnose any illness or disease. We aim to provide the highest quality information, so if you have any questions on the information above, we welcome your feedback!
I
RESOURCES
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Bunions: Overview. 2018 Jun 28. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513134/
- Patient Preference and Physical Demand for Hands-Free Single Crutch vs Standard Axillary Crutches in Foot and Ankle Patients. Kevin D. Martin, DO, Alicia M. Unangst, DO, Jeannie Huh, MD, Jamie Chisholm, MBA. Foot Ankle Int. 2019 Oct;40(10):1203-1208. Epub 2019 Aug 2.
- Unilateral Versus Bilateral Same-Day Surgery Outcomes for Hallux Valgus: An Eight Year Prospective Cohort Study By Jill Dawson, DPhil, Michele Peters, PhD, Crispin Jenkinson, DPhil, Helen Doll, DPhil, Grahame Lavis, BSc (Hons), Robert Sharp, MA FRCS (Ortho), Mark Rogers, FRCS (Ortho), Paul Cooke, ChM FRCS, The Foot and Ankle Online Journal (11): 2 2012.
- Wiley, Blackwell. “Prevalence of bunions increases with age; more common in women.” ScienceDaily. ScienceDaily, 25 February 2011.
- Abbate, Skya. “The Relationship Between Bunions, Sugar, and the Spleen.” Acupuncture Today, Nov. 2012, Vol. 3, Issue 11. http://www.acupuncturetoday.com/mpacms/at/article.php?id=28075
- Ioli, James. “What to Do About Bunions.” Harvard Women’s Health Watch, June 2011. Web. 25 Feb. 2013. http://www.health.harvard.edu/newsletters/Harvard_Womens_Health_Watch/2011/June/what-to-do-about-bunions
- Kristen. “Better Bunion Surgery Recovery.” The Center for Podiatric Care and Sports Medicine, Healing Feet Blog, 27 June 2012. Web. 25 Feb. 2013. http://www.healingfeet.com/blog/foot-care/better-bunion-surgery-recovery
- Mayo Clinic Staff. “Definition of Bunions, Preparing for Your Appointment, Tests and Diagnosis.” The Mayo Clinic. Diseases and Conditions, 25 Jan. 2011. Web. 24 Feb. 2013. http://www.mayoclinic.com/health/bunions/DS00309
- Vanderheiden, Terence. “Metatarsophalangeal Joint.” About.com Guide. Health: Podiatry, 22 May 2011. Web. 27 Feb. 2013. http://foothealth.about.com/od/glossary/g/MTPJ.htm
- Radovic, Phillip A. “Bunions (Hallus Valgus).” MedicineNet.com. Diseases and Conditions: Bunions Article. June 27, 2014. Web. http://www/medicinenet.com