Lower Leg Injury Resource Center
Ankle Replacement
Causes, Treatments, Surgery and Recovery
Ankle replacement surgery, also called ankle arthroplasty, replaces a worn-out ankle joint with an ankle prosthesis. It’s generally used to treat arthritis that has caused long-term debilitating pain and may be considered instead of ankle fusion.
Ankle replacement is a complex operation that’s usually only performed when other treatments have failed.
I
WHAT IS ANKLE REPLACEMENT?
Total ankle replacement is a surgical procedure that removes a worn-out ankle joint and replaces it with a prosthesis made of metal and plastic. The goal of ankle replacement surgery is to relieve pain associated with an arthritic or injured joint while maintaining motion.
Ankle replacement is an alternative to ankle fusion, a procedure that permanently bonds ankle bones together. Ankle fusion was more common historically, but ankle replacement is growing in popularity as prosthetic joints become more reliable and deliver better long-term results.
I
COMMON CAUSES OF ANKLE REPLACEMENT
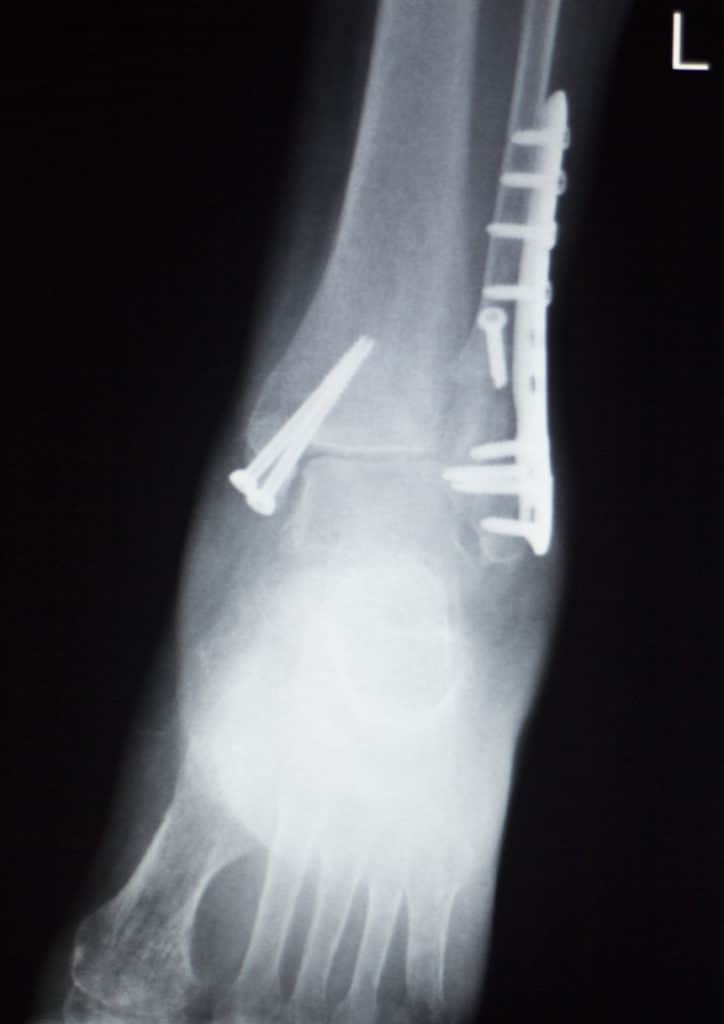
Ankle replacement surgery is usually caused by arthritis that results from an injury like an ankle or talus fracture, dislocation or multiple sprains. This is called post-traumatic arthritis and is seven times more likely in an injured joint than one that is uninjured.
Both osteoarthritis that forms from wear and tear over time and rheumatoid arthritis triggered by an immune response can cause debilitating ankle pain, but osteoarthritis is more common [2].
Ankle replacement surgery is usually performed as a last resort when other treatments haven’t worked. If you have arthritis in your ankle, your doctor will encourage non-surgical options first. Non-surgical treatments include anti-inflammatory medicines, using a brace or cane, shoe inserts, cortisone injections, and physiotherapy.
If non-surgical options fail and ankle pain is affecting your daily life, it may be time to consider surgery. Ankle replacement isn’t for everyone, so your doctor will consider your circumstances carefully.
Ankle replacement surgery is a complicated procedure and isn’t suitable for everybody. Your age, weight, current ankle stability, infection record and preexisting nerve damage are just a few of the factors that will be taken into consideration to determine your suitability..
I
ANKLE REPLACEMENT TREATMENT & SURGERY
Total ankle replacement, also known as ankle arthroplasty, is carried out under general anesthetic or nerve block. Your surgeon will make an incision at the front or side of your ankle to expose the joint and cut away worn surfaces of your shin bone, called the tibia, and uppermost foot bone, called the talus. Your surgeon will replace those surfaces with a prosthetic joint made of metal and plastic. This will help the joint move freely when compared with ankle fusion surgery, which bonds the ankle bones.
Ankle Fusion vs Ankle Replacement
Ankle fusion used to be the gold standard surgical procedure to treat severe ankle arthritis, but advancements in technology in the last two decades have made ankle replacement more reliable and safe.
Your doctor will discuss the options and help you decide which surgery is right for you. In general, ankle fusion puts more stress on nearby joints and can put them at higher risk of developing arthritis, while ankle replacement retains mobility and doesn’t impact nearby joints as much but has a time horizon as short as 10 to 15 years. Recent medical studies indicate recommendations for one or the other should be made on a case-by-case basis.
A 2019 medical study [3] compared patients with ankle replacements and ankle fusions and found no significant differences in outcome. Both groups reported an improvement in joint function, pain relief and quality of life.
I
ANKLE REPLACEMENT RECOVERY TIME
Ankle replacement is a major surgery that will take you off your feet for an extended period. You won’t be able to put any weight on your ankle for six or more weeks, so you’ll need to make adjustments to your usual home and work activities in advance.
Following surgery, your leg will be numb and you may feel discomfort, but your doctor will probably prescribe pain relief medication to help cope during the initial days after surgery. Your incision will be covered by a dressing, and you’ll wear a splint or cast that will protect your ankle while it heals.
You’ll spend between one and three days in the hospital and be discharged when your doctor determines your pain is under control, and you can get around safely with a mobility device.
You won’t be able to put any weight on your ankle for up to six weeks after an ankle replacement. During this time, you’ll need to use a mobility device like crutches, a knee scooter or a hands-free crutch to help you get around.
Choosing a Mobility Device
Following surgery you’ll be asked keep weight off your new ankle for a long period of time. Traditional crutches can be frustrating, painful and exhausting. Fortunately there are more options available to help you stay mobile and active. The most popular crutch alternatives are knee scooters and the iWALK hands-free crutch.
Traditional Crutches
Crutches are the most common mobility device and are used by millions worldwide each year. Designs vary between underarm and elbow crutches, and both styles are relatively cheap and easy to obtain. They can be a useful quick fix to help you get around after surgery.
Crutches can also be frustrating because they require use of your hands and arms, which makes carrying anything or doing most day-to-day chores nearly impossible. Traditional crutches are also exhausting and can cause pain in your hands, arms and shoulders. This generally makes them practical for short distances. It’s not surprising that increasing numbers of people are choosing to use an alternative mobility device.

Knee Scooters or Knee Walkers
A knee scooter is a three- or four-wheeled non-motorized device that allows a user to scoot around with their injured leg resting safely on a padded platform. You use your healthy leg to propel yourself while steering and balancing with your hands using a handlebar. This can make getting around easier, faster and less exhausting than crutches.
Knee scooters are good options for flat surfaces, but they can’t be used on uneven surfaces or stairs, and they are bulky. Perhaps most significantly, they require use of your hands to steer and balance and offer no benefit to a person who wants to carry things or get around on rough or uneven surfaces.

iWALK Hands-Free Crutch
The iWALK hands-free crutch functions like a prosthetic leg, enabling you to walk freely and unaided with full use of your hands and arms. Your injured leg is strapped to a padded platform, which keeps it protected while boosting mobility.
If you’re dreading the idea of being housebound for weeks, the iWALK hands-free crutch could be a great option. It enables you to live your daily life while you recover. It can be used to grocery shop, push a pram, walk the dog, go to work or visit the gym. The iWALK can be used on uneven ground and stairs.
What’s more, studies show that the iWALK hands-free crutch promotes blood flow and prevents atrophy in your injured leg while you heal. This in turn could accelerate healing.

I
WALKING AFTER ANKLE REPLACEMENT
After a period of non-weight bearing activity for your injured foot, you’ll slowly be able to start putting weight on your ankle again. You’ll need physiotherapy to strengthen the joint and increase your range of motion, and you’ll probably continue to wear an orthopedic walking boot for two to four more weeks.
It can take up to a year to fully recover from ankle replacement surgery and get back to normal life. You’ll probably be advised to avoid high-impact activities like running or contact sports but things like swimming, walking and cycling are usually fair game. Talk to your doctor if you have any concerns.
Most ankle replacements last 10 years or more. How long yours will last will depend on a number of factors including how damaged your ankle joint was to begin with, how successful the surgery was, your activity levels, and your overall health.
I
ANKLE REPLACEMENT SURGERY FAQ
Are ankle replacements successful?
New technology is improving the success rate of ankle replacement surgery. Recent studies have documented [4] success rates of 90 percent 10 years after surgery. Swedish research [5] found that 71 percent of patients were either satisfied or very satisfied 24 months after surgery, and 12 percent were dissatisfied or very dissatisfied.
What is the recovery time for an ankle replacement?
You won’t be able to put weight on your ankle for up to six weeks after surgery, and you’ll probably be asked to wear an orthopedic walking boot when you do start walking.
People recover at different speeds, so go at your doctor’s recommended pace. Physiotherapy can help, so make sure you perform the exercises prescribed by your therapist. It can take up to a year before you fully recover from ankle replacement surgery.
What is replaced in an ankle replacement?
The ankle is where your shinbone, called the tibia, and upper foot bone, called the talus, meet. During ankle replacement, the surgeon will remove damaged portions of the joint and replace them with a new prosthetic joint made of metal and plastic.
What happens when an ankle replacement wears out?
Research shows that 90 percent of artificial ankles are still functioning well 10 years after surgery. They can loosen or wear out over time, however. If this happens you may need another surgery or to consider ankle fusion surgery, which bonds the bones of your ankle together.
Is ankle replacement covered by medical insurance?
The total cost of ankle replacement surgery can be around $40,000. The procedure is covered by Medicare, but as of 2009 some health insurance companies still declined to pay for it, deeming the procedure experimental. There may be certain criteria you must meet for your insurer to cover it.
How long does ankle surgery take?
Ankle replacement surgery usually takes two to two and a half hours. The non-weight bearing portion of recovery can take six to eight weeks. Total recovery can take up to a year.
How do you treat arthritis in the ankle?
Ankle arthritis is often caused by a previous injury, such as a broken ankle, but it can also result from osteoarthritis or rheumatoid arthritis. The main symptoms are swelling, pain, stiffness, and a reduced ability to walk. If you have arthritis in your ankle, you’ll be encouraged to try non-surgical treatment first. This may include:
- Wearing orthotic shoe inserts or custom-made shoes
- Taking nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen
- Using a cane or wearing a brace
- Physiotherapy to help increase range of motion and flexibility
- Cortisone injections
Can arthritis be removed from your ankle?
The aim of non-surgical treatment is to reduce the symptoms of arthritis in your ankle. If these don’t work and your symptoms impact your daily activity, surgery may be recommended to remove part of the arthritic joint. Your doctor will assess your case individually to determine whether total ankle replacement or ankle fusion is right for you.
What is end stage ankle arthritis?
End stage ankle arthritis is when the surfaces of bone in the ankle joint have been progressively worn down and cause pain, loss of function and loss of mobility—severely limiting daily activity. If you’re diagnosed with end-stage ankle arthritis, and non-surgical treatments haven’t helped, you may be advised to consider surgery.
The information above is intended for informational purposes only and is not intended to prevent, treat, or diagnose any illness or disease. We aim to provide the highest quality information, so if you have any questions on the information above, we welcome your feedback!
- Goldberg AJ, Zaidi R, Thomson C, Doré CJ, Skene SS, Cro S, Round J, Molloy A, Davies M, Karski M, Kim L, Cooke P; TARVA study group. Total ankle replacement versus arthrodesis (TARVA): protocol for a multicentre randomised controlled trial. BMJ Open. 2016 Sep 6;6(9) https://www.ncbi.nlm.nih.gov/pubmed/27601503
- Valderrabano, V., Horisberger, M., Russell, I., Dougall, H., & Hintermann, B. (2009). Etiology of ankle osteoarthritis. Clinical orthopaedics and related research, 467(7), 1800–1806. https://doi.org/10.1007/s11999-008-0543-6
- Wąsik, J., Stołtny, T., Pasek, J., Szyluk, K., Pyda, M., Ostałowska, A., Kasperczyk, S., & Koczy, B. (2019). Effect of Total Ankle Arthroplasty and Ankle Arthrodesis for Ankle Osteoarthritis: A Comparative Study. Medical science monitor : international medical journal of experimental and clinical research, 25, 6797–6804. https://doi.org/10.12659/MSM.915574
- Barg, A., Wimmer, M. D., Wiewiorski, M., Wirtz, D. C., Pagenstert, G. I., & Valderrabano, V. (2015). Total ankle replacement. Deutsches Arzteblatt international, 112(11), 177–184. https://doi.org/10.3238/arztebl.2015.0177
- Kamrad, I., Carlsson, Å., Henricson, A., Magnusson, H., Karlsson, M. K., & Rosengren, B. E. (2017). Good outcome scores and high satisfaction rate after primary total ankle replacement. Acta orthopaedica, 88(6), 675–680. https://doi.org/10.1080/17453674.2017.1366405
The Best Mobility Device
for Ankle Replacements.
The Best Mobility Device
for Ankle Replacements.
Free 1-2 Day Delivery
to most locations



